Gastric BypassOr ‘My stomach shrank
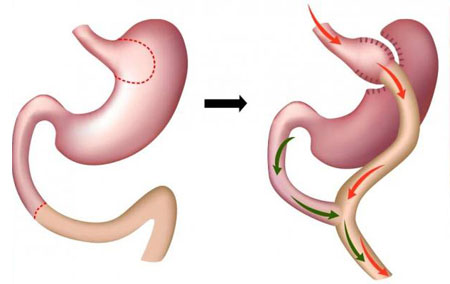
Gastric bypass surgery is the most commonly preferred method in the treatment of obesity, or as people call it, excessive obesity. We can define “morbid obesity” as excessive and diseased obesity. Gastric bypass is a surgical procedure used in the treatment of morbid obesity, where excess weight turns into fat tissue in the body and causes different health problems.
With gastric bypass surgery, diseases such as diabetes, high blood pressure and bad cholesterol caused by excess weight can be more easily controlled.
Gastric Bypass surgery is a procedure that provides weight loss by both reducing or restricting the stomach capacity and disabling a certain part of the small intestines. Gastric bypass is a surgery that is applied to reduce the absorption of fatty and carbohydrate foods from the intestines.
“My stomach shrank”
You know, when we talk among ourselves, we say "my stomach has shrunk" to explain that our appetite has decreased, in fact, this is exactly what happened after gastric bypass surgery.
Yes, with this surgery, 90% of the patient's stomach is disabled. The remaining 10% of the stomach is connected to 150 cm ahead of the small intestine and the surgery is completed. After gastric bypass surgery, the nutrients taken go to 10% of the stomach, and thanks to the tension in the stomach wall of this small section, a feeling of early satiety occurs. With the transfer of food to the middle part of the small intestine, carbohydrates, sugars and fats are eliminated from the body without being absorbed in the small intestines, that is, without mixing with the blood.
What are the Types of Gastric Bypass Surgery?
This surgical operation is divided into two as Gastric Bypass surgery and Mini Gastric Bypass surgery.
The common purpose of gastric bypass surgeries is to shrink the stomach and ensure that the consumed foods reach the intestines faster. Thus, two birds are hit with one stone, and both targets are achieved.
The first goal is for the patient to have a feeling of fullness more easily by shrinking the stomach. The second goal is the rapid passage of food into intestinal digestion. Thus, more calories and much less weight gain is provided.
In mini gastric bypass surgeries, no part of the body is cut. Therefore, the patient recovers quickly.
In order to reduce the current caloric value of the foods taken with this operation, a shorter route is drawn directly to the stomach - small intestine. In fact, this is the goal of normal gastric bypass surgery.
So what is the difference between the two?
The most obvious difference is that nothing is removed from the body.
After the mini gastric bypass surgery, the obese patient stays in the hospital for at least two and at most four days and is discharged.
To Whom Gastric Bypass Surgery Is Applied?
People with a BMI between 35-40 and a disease that develops due to being overweight (Hypertension, heart disease, Type-2 diabetes, sleep apnea, joint disease, etc.),
Patients aged 18-65 years,
Those who are obese but cannot lose weight with diet and exercise,
Those who can tolerate surgery and anesthesia,
These can undergo Gastric Bypass surgery.
Who Cannot Have Gastric Bypass Surgery?
Those with serious and untreated psychiatric illness,
Those with substance or alcohol addiction,
Patients with severe hormonal disorders,
Patients who cannot make the necessary changes in diet and lifestyle after surgery,
Those who have a disease that will prevent them from receiving anesthesia,
Cancer patients,
Those planning a pregnancy within 1 year,
These cannot have gastric bypass and bariatric and metabolic surgery operations.
What are the Test to be Conducted Before Gastric Bypass Surgery?
Before Gastric Bypass surgery, patients are evaluated with some tests.
The tests to be conducted are as follows:
Blood and biochemistry tests
Hormone tests
Hemogram
Hepatitis tests
Whole abdominal USG
Gastric endoscopy
Lung X-ray
Heart X-ray (ECG)
Lung breathing test
If necessary, stress testing and electrocardiography
After all these tests, all necessary examinations and screenings are carried out by specialists from anesthesia, internal medicine, cardiology, chest diseases and endocrine units. If there is a condition that prevents the patient from undergoing surgery, it is checked, and a possible underlying disease that will cause weight gain after surgery is determined. The steps to be taken before and after the treatment are carefully planned within the approval and recommendations of the experts.
How Gastric Bypass Surgery Is Performed?
Thanks to today's modern surgical methods, these operations are now routinely performed with laparoscopic surgery. In laparoscopic surgery, your abdomen is not opened to reach the operating area. Surgery is performed with the support of advanced technology, without major cuts or wounds.
Although laparoscopy is the most frequently used method as a routine procedure today, robotic surgery is also an alternative surgical method.
Rarely, these surgeries are also performed with open surgery. Open surgery is a method that can be applied after any problems that may arise during laparoscopy or robotic surgery.
It should be noted that every closed method (Laparoscopic or Robotic) has the potential to switch to open surgery to a certain extent.
This operation, which is performed to reduce the volume of the stomach and to restrict absorption, is two-stage. In the first stage of the operation performed with the closed method, a small stomach tube with a volume of 30 ml is created at the entrance of the stomach and the remaining large stomach is completely separated. This large stomach is removed from the abdomen and continues to produce its secretions. In the second stage, a connection is made to the small stomach tube with the small intestine. Through this connection, nutrients bypass the large stomach and work by passing into the small intestine. As a result of this process, it limits the amount of food consumed. Thus, it may be possible to see weight loss as a result of less food and less absorption.
There are two types of this method of restricting food intake. The process of connecting the small intestines to the stomach in the form of a ring without separating them is called mini gastric bypass. In Roux en Y gastric bypass, the small intestine is separated and one end is connected to the stomach and the other end to the small intestine from a certain distance. Both of these processes contribute to weight loss with similar results. In short, after this procedure, the patient consumes less food and can benefit less from the food he consumes.
Gastric bypass surgery can give more significant results compared to sleeve gastrectomy.
The feeling of hunger decreases and the feeling of satiety increases. As a result, the person's blood sugar is also stable. Since it is a method that restricts food intake after the operation, 60 to 80% of the person's excess weight can be lost. However, gastric bypass procedure has a higher complication rate compared to sleeve gastrectomy, and long-term or life-long medication may be required after the procedure.
What are the Advantages of Gastric Bypass Surgery?
After Gastric Bypass surgery, long-term weight control can be achieved with small portions without a strong sense of appetite.
For most patients, long-term weight loss and weight maintenance is successful. Depending on weight loss, permanent solutions emerge for concomitant diseases caused by obesity, especially Type 2 diabetes. After the surgery, patients experience physical and psychological satisfaction.
What are the Disadvantages of Gastric Bypass Surgery?
Longer hospital stay.
At least two vitamin and mineral supplements are required for life, as it causes malabsorption. Severe vitamin deficiency syndrome may occur if vitamins are not used.
Gastric Bypass is a more complicated and longer-lasting surgery, so the complication rates are higher.
Requires closer follow-up.
Dumping syndrome may occur.
The stomach remains in the abdomen, which cannot be visualized by endoscopy.
Problems such as intestinal obstruction and ulcers may occur after gastric bypass surgery.
How Nutrition Should Be After Gastric Bypass Surgery?
After surgery, a diet under the control of a dietitian is recommended.
Liquid purees are consumed for the first 6-8 weeks.
Step by step, a normalization is achieved in the nutrition process.
Within 3 to 6 months, a new diet is started in line with the patient's health.
During this process, patients can take supplements such as vitamins, minerals and calcium.




